Overview
Trigger finger makes a finger get stuck in a bent position. It may straighten suddenly with a snap. The fingers most often affected are the ring finger and the thumb, but the condition can affect any finger.
Trigger finger happens when the tendon that controls that finger can't glide smoothly in the sheath that surrounds it. This may occur if part of the tendon sheath becomes swollen or if a small lump forms on the tendon.
The condition is most common in women over the age of 50. You may be at higher risk of trigger finger if you have diabetes, low thyroid function or rheumatoid arthritis.
Treatment of trigger finger can include splinting, steroid injections or surgery.
Symptoms
Symptoms of trigger finger may progress from mild to severe and include:
- Finger stiffness, particularly in the morning.
- A popping or clicking sensation as the finger moves.
- Tenderness or a bump in the palm at the base of the affected finger.
- Finger catching or locking in a bent position, which suddenly pops straight.
- Finger locked in a bent position.
Trigger finger can affect any finger, including the thumb. More than one finger may be affected at a time, and both hands might be involved. Triggering is usually worse in the morning.
Causes
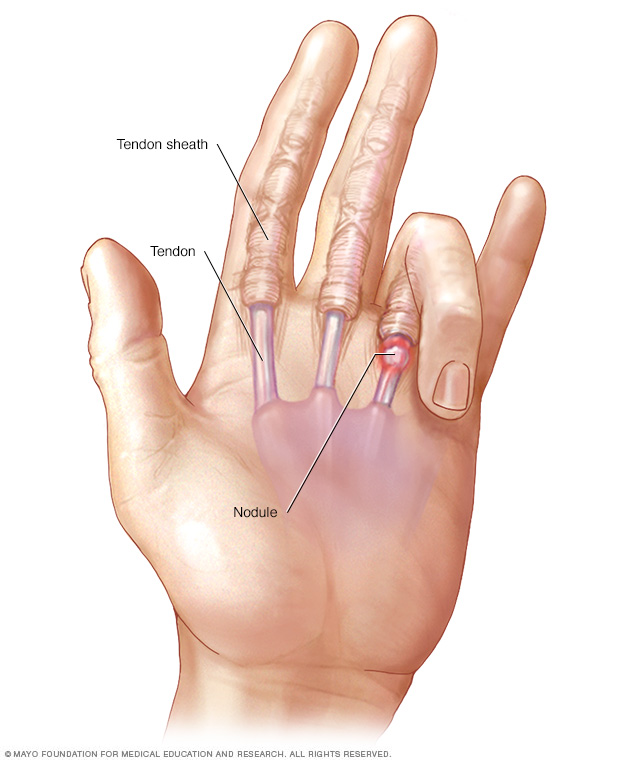
Tendons are tough cords that attach muscle to bone. Each tendon is surrounded by a protective sheath. Trigger finger occurs when the affected finger's tendon sheath becomes irritated and swollen. This makes it harder for the tendon to glide through the sheath.
In most people, there's no explanation for why this irritation and swelling begins.
The constant back-and-forth irritation can cause a small lump of tissue to form on the tendon. This lump is called a nodule. The nodule can make it even harder for the tendon to glide smoothly.
Risk factors
Factors that put you at risk of developing trigger finger include:
- Repeated gripping. Occupations and hobbies that involve repetitive hand use and prolonged gripping may increase the risk of trigger finger.
- Certain health problems. People who have diabetes or rheumatoid arthritis are at higher risk of developing trigger finger.
- Your sex. Trigger finger is more common in women.
Complications
Trigger finger can make it harder to type, button a shirt or insert a key into a lock. It also can affect your ability to grip a steering wheel or grasp tools.
Diagnosis
During the exam, a health care provider may ask you to open and close your hand, checking for areas of pain, smoothness of motion and evidence of locking.
Treatment
Trigger finger treatment varies depending on its severity and duration.
Medications
Consider taking a nonsteroidal anti-inflammatory drug, such as ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve). Some types of these medicines can be delivered by creams or patches through the skin right where the problem is happening.
Therapy
Conservative noninvasive treatments may include:
- Rest. Avoid activities that require repetitive gripping, repeated grasping or the prolonged use of vibrating hand-held machinery until your symptoms improve. If you can't avoid these activities altogether, padded gloves may offer some protection.
- A splint. Wearing a splint can help rest the tendon.
- Stretching exercises. Gentle exercises can help maintain mobility in your finger.
Surgical and other procedures
If your symptoms are severe or if conservative treatments haven't helped, your health care provider might suggest:
- Steroid injection. An injection of a steroid near or into the tendon sheath may reduce inflammation and allow the tendon to glide freely again. An injection is often effective for more than a year. Some people need more than one injection.
- Needle procedure. After numbing your palm, a member of your care team inserts a sturdy needle into the tissue around your affected tendon. Moving the needle and your finger helps break apart the tissue that's blocking the smooth motion of the tendon. Using ultrasound guidance during the procedure can improve results.
- Surgery. Working through a small incision near the base of your affected finger, a surgeon can cut open the narrowed section of tendon sheath.
Preparing for an appointment
You'll probably start by seeing your primary care doctor to determine what could be causing your symptoms.
What you can do
Make sure to bring a list of all the medications and supplements you take regularly. You also might want to write down some questions in advance. Examples may include:
- What's causing my symptoms?
- Is this condition temporary or long lasting?
- What treatments are available?
- Are there complications associated with this condition or its treatments?
What to expect from your doctor
Your health care provider is likely to ask you a number of questions. Being ready to answer them may reserve time to go over important information a second time.
Questions your provider might ask include:
- What symptoms are you experiencing?
- How long have you been experiencing these symptoms?
- Do your symptoms seem to come and go, or do you always have them?
- Does anything seem to make your symptoms better?
- Does anything seem to make your symptoms worse?
- Are your symptoms worse in the morning or at any particular time of the day?
- Do you perform repetitive tasks on the job or for hobbies?
- Have you recently experienced any injury to your hand?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


