Overview
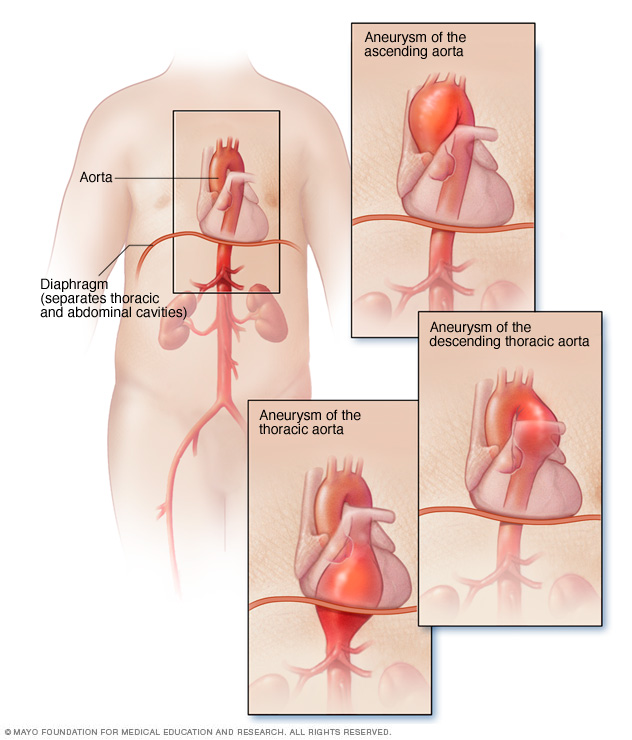
A thoracic aortic aneurysm is a weakened area in the body's main artery in the chest. The body's main artery is called the aorta. When the aortic wall is weak, the artery may get wider. When the artery gets very wide, it's called an aneurysm. An aneurysm can happen anywhere in the thoracic aorta, including near the heart.
A thoracic aortic aneurysm also is called a thoracic aneurysm. If the aneurysm is between the upper and lower parts of the aorta, it's called a thoracoabdominal aneurysm.
Thoracic aortic aneurysms are less common than aneurysms in the lower part of the aorta, called abdominal aortic aneurysms.
Treatment of a thoracic aortic aneurysm depends on the cause and size of the aneurysm and how fast it's growing. Treatment may range from regular health checkups to emergency surgery. A thoracic aortic aneurysm that ruptures or causes a tear called a dissection is a medical emergency that can lead to death.
Symptoms
Thoracic aortic aneurysms often grow slowly. There are usually no symptoms. That makes them hard to find. Many start small and stay small. Others get bigger over time. How quickly a thoracic aortic aneurysm may grow is hard to predict.
As a thoracic aortic aneurysm grows, symptoms may include:
- Back pain.
- Cough.
- Weak, scratchy voice.
- Shortness of breath.
- Tenderness or pain in the chest.
Symptoms that a thoracic aortic aneurysm has ruptured or caused a tear called an aortic dissection include:
- Sharp, sudden pain in the upper back that spreads down the body.
- Pain in the chest, jaw, neck or arms.
- Trouble breathing.
- Low blood pressure.
- Loss of consciousness.
- Shortness of breath.
- Trouble swallowing.
Some aneurysms may never rupture or lead to dissection.
When to see a doctor
Most people with thoracic aortic aneurysms don't have symptoms until an aortic dissection or rupture occurs. An aortic dissection or aneurysm rupture is a medical emergency. Call 911 or your local emergency number for immediate help.
Causes
Causes of thoracic aortic aneurysms may include:
- Atherosclerosis. A buildup of fats, cholesterol, and other substances in and on the artery walls causes the arteries to get stiff. Over time, the walls of the arteries may get weak. High blood pressure and high cholesterol increase the risk of atherosclerosis, especially in older people.
-
Genetic conditions. Aortic aneurysms in younger people are often caused by changes in genes. A genetic condition called Marfan syndrome can weaken the wall of the aorta.
If you have Marfan syndrome or a related condition, such as Loeys-Dietz syndrome or vascular Ehlers-Danlos syndrome, you have a much higher risk of a thoracic aortic aneurysm. These conditions also make you more likely to have an aortic rupture or aortic dissection.
- Blood vessel inflammation. Conditions that cause irritation and swelling of blood vessels, such as Takayasu arteritis and giant cell arteritis, are associated with thoracic aortic aneurysms.
- Bicuspid aortic valve. Usually the valve between the lower left heart chamber and the aorta has three flaps. A bicuspid valve has only two. People who are born with a bicuspid aortic valve are more likely to get a thoracic aneurysm.
- Untreated infection. Though rare, it's possible to get a thoracic aortic aneurysm if you've had an untreated infection such as syphilis or salmonella.
- Traumatic injury. Some people who are injured in falls or motor vehicle crashes get thoracic aortic aneurysms. But this is rare.
Risk factors
Anything that damages or weakens blood vessels may raise the risk of an aneurysm. Thoracic aortic aneurysm risk factors include:
- Age. Thoracic aortic aneurysms occur most often in people age 65 and older.
- Smoking and tobacco use. If you smoke or chew tobacco, it's important that you quit. Using tobacco also can worsen an aneurysm and overall health.
- High blood pressure. Increased blood pressure damages the blood vessels in the body. This raises the risk of an aneurysm.
- Coronary artery disease. This type of heart disease causes reduced blood flow to the heart. It's often caused by atherosclerosis. Atherosclerosis can damage the lining of a blood vessel, increasing the risk of an aneurysm. This is a more common risk in older people.
- Family history. You're more likely to get an aortic aneurysm and rupture if you have a parent, brother, sister or child with one. You may develop aneurysms at a younger age.
If you're at risk of an aortic aneurysm, you might get medicines to lower your blood pressure and relieve stress on weakened arteries.
Complications
Possible complications of a thoracic aortic aneurysm are:
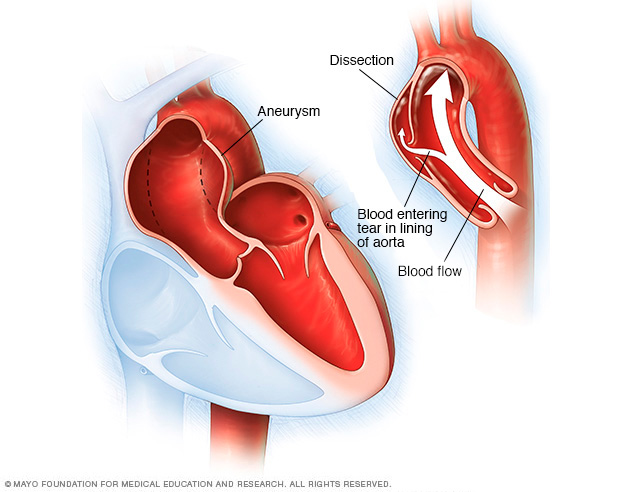
- A tear in the wall of the aorta, also called an aortic dissection. This life-threatening condition causes bleeding into and along the aortic wall. Emergency surgery is needed to prevent death.
- Rupture of the body's main artery, called an aortic rupture. If a tear in the aorta causes bleeding outside the aorta, it's called an aortic rupture. This also is a life-threatening condition that needs treatment right away. In general, the larger the aneurysm, the greater the risk of rupture.
- Blood clots. Small blood clots can develop in the area of the aortic aneurysm. If a blood clot breaks loose from the inside wall of an aneurysm, it can block a blood vessel elsewhere in the body. This can possibly cause serious complications.
- Stroke. Signs and symptoms of stroke include weakness of or an inability to move one side of the body. It may be hard to speak.
Prevention
To prevent an aneurysm, keep the blood vessels as healthy as possible. Try these healthy lifestyle tips.
- Don't smoke or use tobacco.
- Control blood pressure and cholesterol levels.
- Keep a healthy weight and stay active.
- Eat nutritious foods.
Screening
Screening means that you have regular imaging tests, usually an echocardiogram, to look for an aneurysm.
Your healthcare professional may suggest screening for a thoracic aneurysm if:
- You have a parent, brother, sister, son or daughter with a genetic condition linked to thoracic aortic aneurysms. An example is Marfan syndrome.
- You have a family history of aortic aneurysms and wish to get pregnant.
If a screening test shows a larger than usual aorta or an aneurysm, the test is usually repeated within 6 to 12 months to look for changes.
Diagnosis
Thoracic aortic aneurysms often don't have symptoms. So they can be hard to diagnose. They are often found when an imaging test is done for a different reason.
If you have a thoracic aortic aneurysm, your healthcare professional may ask about your family's medical history. Some aneurysms can run in families.
Tests
Tests are done to diagnose or screen for a thoracic aortic aneurysm. Tests may include:
- Echocardiogram. Sound waves show how blood moves through the heart and blood vessels, including the aorta. This test may be used to diagnose or screen for thoracic aortic aneurysms. A standard echocardiogram looks at the aorta from outside the body. If it doesn't give enough details, a transesophageal echocardiogram may be done. This type looks at the aorta from inside the body.
- CT scan. X-rays make cross-sectional images of the body, including the aorta. This test can show the size and shape of an aneurysm.
- Heart MRI, also called a cardiac MRI. A magnetic field and radio waves create pictures of the heart and aorta. A heart MRI can diagnose an aneurysm and show its size and location. This test doesn't use radiation. It may be an option to CT scans for people who need frequent imaging tests.
Treatment
The goals of treatment for a thoracic aortic aneurysm are to:
- Stop the aneurysm from growing.
- Prevent aortic rupture.
Treatment depends on the aneurysm's size and how fast it's growing.
Treatment for thoracic aortic aneurysm may include:
- Regular health checkups, sometimes called watchful waiting.
- Medicines.
- Surgery.
Regular checkups
Small thoracic aneurysms may only need medicine and regular imaging tests to watch the aneurysm.
Usually you get an echocardiogram, CT or magnetic resonance angiography scan at least six months after your aneurysm is diagnosed. How often you need these tests depends on the cause and size of the aneurysm, and how fast it's growing.
Medications
Medicines may be used to treat high blood pressure, high cholesterol and other conditions linked to aneurysms.
- Beta blockers. These medicines slow the heartbeat and lower blood pressure. They may reduce how fast the aorta is widening in people with Marfan syndrome.
- Angiotensin 2 receptor blockers (ARBs). These medicines may be used if beta blockers can't be taken or if they don't lower blood pressure enough. They are often recommended for people who have Loeys-Dietz syndrome even if they don't have high blood pressure. Examples of ARBs include losartan (Cozaar), valsartan (Diovan) and olmesartan (Benicar).
- Statins. These medicines help lower cholesterol. They can help reduce the risk of blockages in the arteries and aneurysm complications. Examples of statins are atorvastatin (Lipitor), lovastatin (Altoprev), simvastatin (Zocor, FloLipid) and others.
Surgery or other procedures
Surgery is generally recommended for thoracic aortic aneurysms about 1.9 to 2.4 inches (about 5 to 6 centimeters) and larger. Surgery may be recommended for smaller aneurysms if you have a family history of aortic dissection or a condition linked to aortic aneurysm, such as Marfan syndrome.
The type of surgery done depends on:
- The cause of the aneurysm.
- Your overall health.
- The location of the aneurysm.
Types of surgeries and procedures for thoracic aortic aneurysms include:
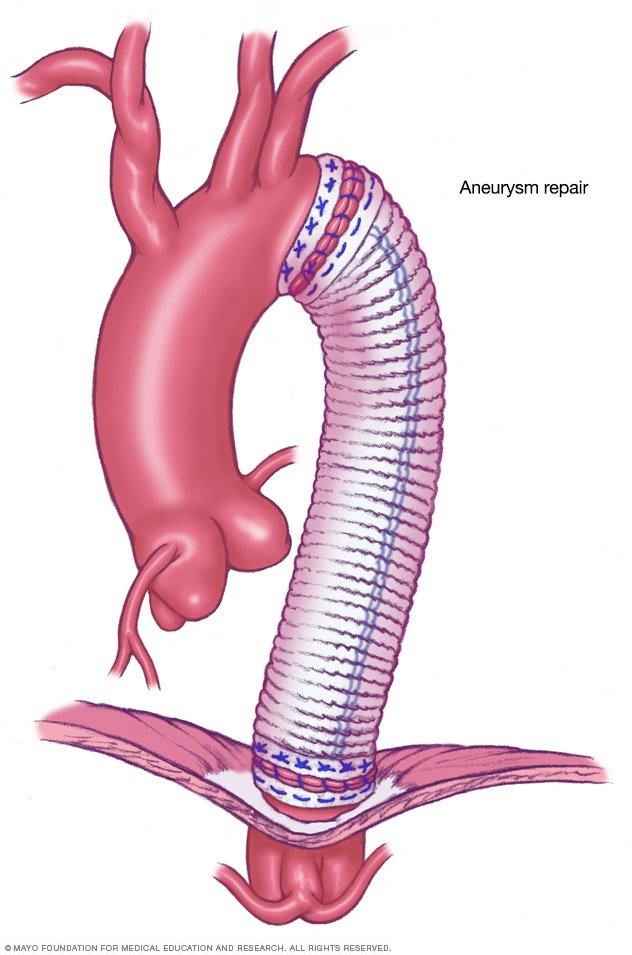
- Open surgery. Most people with a thoracic aortic aneurysm have this major surgery. A surgeon removes part of the aorta damaged by the aneurysm. It's replaced with a tube, called a graft, which is sewn into place.
- Aortic root surgery. This surgery is done to prevent an aortic aneurysm from rupturing. A surgeon takes out part of the aorta and sometimes the aortic valve. A graft replaces the removed part of the aorta. The aortic valve may be replaced with a mechanical or biological valve. If the valve is not removed, the surgery is called valve-sparing aortic root repair.
-
Endovascular aortic aneurysm repair (EVAR). This treatment is a less invasive option to open surgery. That means it uses small surgical cuts and may allow a faster recovery. The surgeon places a thin, flexible tube into a blood vessel, usually in the groin, and guides it to the aorta. A graft on the end of the catheter goes where the aneurysm is. Small hooks or pins hold the graft in place. The graft strengthens the weakened part of the aorta.
EVAR can't be done on everyone. Ask your healthcare professional whether it's right for you. After EVAR, you need regular imaging tests to make sure the graft is working correctly.
- Emergency surgery. A ruptured thoracic aortic aneurysm needs emergency surgery. This open-chest surgery is risky. There is a high chance of complications. That's why it's important to find and treat thoracic aortic aneurysms before they rupture.
Lifestyle and home remedies
If you have a thoracic aortic aneurysm, your healthcare team may tell you not to do heavy lifting. You also might be told not to do some energetic physical activities. Such activities can increase blood pressure. High blood pressure can put pressure on an aneurysm.
If you want to do a particular activity, talk with your healthcare team. You may need an exercise stress test to see how activity affects your blood pressure. Moderate physical activity is generally healthy.
Emotional stress also can raise blood pressure. It's important to manage or lower stress. Some tips are to get more exercise and practice mindfulness.
Coping and support
You may find that connecting with others who have experienced similar situations may be helpful. Ask your healthcare team about support groups in your area.
Preparing for an appointment
If you have a family history of thoracic aortic aneurysms or conditions linked to them, make an appointment for a health checkup. If an aneurysm is found early, treatment may be easier and more effective.
Appointments can be brief and there's often a lot to talk about. So it's a good idea to be prepared. Here's some information to help you get ready for your appointment.
What you can do
- Ask if there's anything you need to do to prepare. For example, you may be told not to eat or drink for a while before some tests.
- Write down your symptoms. Include any that may seem unrelated to a thoracic aortic aneurysm.
- Write down important personal information, including a family history of heart disease, aneurysms or connective tissue disease.
- Make a list of all medicines, vitamins or supplements that you take. Include dosages.
- Take someone along, if possible. It can be hard to remember the information given to you during an appointment. Someone who goes with you may remember something that you missed or forgot.
- Be prepared to talk about your diet, exercise habits and tobacco use. If you don't already follow a diet or exercise routine, tell your healthcare professional about any challenges you might face in getting started. Be sure to tell your healthcare team if you smoke or have ever smoked.
- Send imaging reports and bring records. It's helpful if you can send imaging reports to your healthcare professional in advance. Bring your medical records.
- Write down questions to ask your healthcare professional.
For a thoracic aortic aneurysm, some basic questions to ask your healthcare professional are:
- What tests do I need?
- What size is my aneurysm?
- What treatments are available, and which do you recommend for me?
- What's an appropriate level of physical activity?
- Do I need to change my diet?
- How often should I be screened for an aneurysm?
- Should I tell other family members to be screened for an aneurysm?
- I have other health conditions. How can I best manage these conditions together?
- Is there any information that I can take home with me? What websites do you recommend?
Don't hesitate to ask any other questions.
What to expect from your doctor
Your healthcare team usually asks you several questions. Being ready to answer them may save time to go over any points you want to spend more time on. Your healthcare team may ask:
- When did your symptoms start?
- Do your symptoms come and go, or do you have them all the time?
- On a scale of 1 to 10, with 10 being the worst, how bad are your symptoms?
- Do you have a family history of aneurysms or genetic diseases, such as Marfan syndrome?
- Do you smoke? Have you ever smoked?
- Have you ever been told that you have high blood pressure?
- What, if anything, make your symptoms better?
- What, if anything, make your symptoms worse?
What you can do in the meantime
Healthy lifestyle changes can help protect the heart and blood vessels. It's never too early to start. Eat healthy foods, stay active and do not smoke. Taking these steps can help prevent thoracic aortic aneurysm and its complications.
If you're diagnosed with a thoracic aortic aneurysm, ask how often you need health checkups.
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


