Overview
Scabies is an itchy skin rash caused by a tiny burrowing mite called Sarcoptes scabiei. Intense itching occurs in the area where the mite burrows. The need to scratch may be stronger at night.
Scabies is contagious and can spread quickly through close person-to-person contact in a family, child care group, school class, nursing home or prison. Because scabies spreads so easily, health care providers often recommend treating the entire family or any close contacts.
Scabies is easily treated. Medicated skin creams or pills kill the mites that cause scabies and their eggs. But itching may not stop for many weeks after treatment.
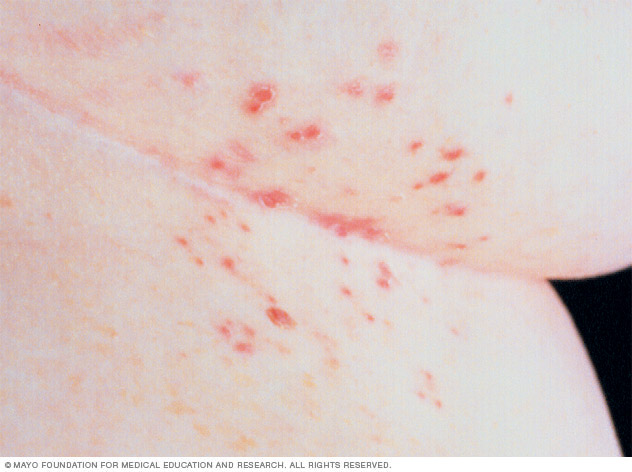
Symptoms
Scabies symptoms include:
- Itching, often severe and usually worse at night
- Thin, wavy tunnels made up of tiny blisters or bumps on the skin
Scabies is often found in the skin folds. But scabies can appear on many parts of the body. In adults and older children, scabies is most often found:
- Between the fingers and toes
- In the armpits
- Around the waist
- Along the insides of the wrists
- On the inner elbows
- On the soles of the feet
- On the chest
- Around the nipples
- Around the belly button
- Around the genitals
- In the groin area
- On the buttocks
In infants and young children, common sites of scabies usually include the:
- Fingers
- Face, scalp and neck
- Palms of the hands
- Soles of the feet
If you've had scabies before, symptoms may start within a few days of exposure. If you've never had scabies, it can take as long as six weeks for symptoms to start. You can still spread scabies even if you don't have any symptoms yet.
When to see a doctor
Talk to your health care provider if you have any symptoms of scabies.
Many skin conditions, such as dermatitis or eczema, also can cause itching and small bumps on the skin. Your health care provider can find the exact cause of your symptoms so that you receive the right treatment. Antihistamines or nonprescription lotions may ease itching. But they won't get rid of the mites or their eggs.
Causes
Scabies is caused by a tiny, eight-legged mite. The female mite burrows just under the skin and makes a tunnel where it lays eggs.
The eggs hatch, and the mite larvae travel to the surface of the skin, where they mature. These mites can then spread to other areas of the skin or to the skin of other people. Itching is caused by the body's allergic reaction to the mites, their eggs and their waste.
Close skin-to-skin contact and, less often, sharing clothing or bedding with a person who has scabies can spread the mites.
Pets don't spread scabies to humans. The scabies mites that affect animals don't survive or reproduce in people.
However, coming in contact with an animal that has scabies may cause brief itching if the mite gets under the skin. But within a few days, the mite will die. So treatment isn't needed.
Complications
Scratching too much can break your skin and cause an infection, such as impetigo. Impetigo is an infection on the skin's surface that's caused most often by staph bacteria (staphylococci) or sometimes by strep bacteria (streptococci).
A more severe type of scabies, called crusted scabies, may affect certain people, including:
- Young children
- People with developmental disabilities
- People with weakened immune systems, such as those with HIV or lymphoma, or people who have had organ transplants
- People who are very sick, such as people in hospitals or nursing facilities
- Older people in nursing homes
Crusted scabies makes the skin crusty and scaly, and affects large areas of the body. It's very contagious and can be hard to treat. Quick treatment with both a prescription pill and a skin cream is needed.
Typically, someone with scabies has about 10 to 15 mites. But someone with crusted scabies may have millions of mites. Yet itching may not occur or may be mild.
Prevention
To prevent scabies from coming back and to keep the mites from spreading to other people, take these steps:
- Wash all clothes and linen. Heat kills the mites and their eggs. Use hot, soapy water to wash all clothing, towels and bedding used in the last three days before beginning treatment. Dry with high heat. Dry-clean items you can't wash at home.
- Starve the mites. Place items you can't wash in sealed plastic bags and leave them in an out-of-the-way place, such as your garage, for a week. Mites die after a few days without food.
- Clean and vacuum. It's a good idea to clean your home to prevent scabies from spreading. This is especially true for people with crusted scabies. Vacuum furniture, carpets and floors to remove scales and crusts that may have scabies mites.
Diagnosis
To diagnose scabies, your health care provider looks at your skin for symptoms of mites. Your provider may also take a sample of your skin to look at under a microscope. This allows your provider to see if any mites or eggs are present.
Treatment
Scabies treatment involves killing the mites and eggs with a medicated cream or pill. No treatment is available without a prescription. Several creams and lotions are available by prescription.
Your health care provider will likely ask you to apply the medication to your whole body, from the neck down. You'll need to leave it on for at least 8 to 14 hours. Sometimes, you may have to apply the lotion twice. More treatments may be needed if new symptoms appear..
Because scabies spreads so easily, your health care provider will likely recommend treating all household members and other close contacts, even if they don't have symptoms of scabies..
Treatment for scabies often includes:.
- Permethrin cream. Permethrin is a skin cream with chemicals that kill mites that cause scabies and their eggs. It's generally considered safe for adults, people who are pregnant or breastfeeding, and children over 2 months old.
- Sulfur cream. Sulfur cream is a scabies treatment that can be applied overnight, rinsed off and then reapplied for five nights in a row. Sulfur is safe to use in pregnancy and in children under 2 months old.
- Ivermectin (Stromectol). Ivermectin can be taken as a pill to treat scabies when prescription lotions don't work. It's often prescribed for people with crusted scabies or lowered immune systems. Ivermectin isn't recommended for people who are pregnant or nursing, or for children who weigh less than 33 pounds (15 kilograms).
Although these drugs kill the mites quickly, itching may not stop for many weeks.
Health care providers may prescribe other skin care treatments for people who don't get relief from or can't use these drugs.
Lifestyle and home remedies
Your skin might still itch for several weeks after scabies treatment. Taking oral allergy pills or using nonprescription skin creams, such as calamine lotion, may help ease itching.
Preparing for an appointment
Make an appointment with a member of your health care team if you or your child has symptoms of scabies.
Here's some information to help you get ready for your appointment.
Things to do before your appointment
- List any symptoms you or your child has had, and for how long.
- List any possible sources of infection, such as other family members who have had a rash.
- Write down key medical information, including any other health problems and the names of any medications you or your child is taking.
- Write down questions you want to ask your provider.
Below are some basic questions to ask your provider about scabies.
- What's the most likely cause of these symptoms?
- What treatment do you recommend?
- How soon will my symptoms improve with treatment?
- When will you see me or my child again to be sure the treatment is working?
- Are there any home remedies or self-care steps that I can use to relieve symptoms?
- Am I or is my child contagious? For how long?
- How can I prevent spreading scabies to others?
What to expect from your doctor
Your health care provider is likely to ask you several questions. Preparing for these questions ahead of time may help ensure that you get the most out of your appointment. Your provider may ask:
- What symptoms have you noticed?
- When did you first notice these symptoms?
- Have these symptoms gotten worse over time?
- If you or your child has a rash, what parts of the body are affected?
- Have you been in frequent, close contact with anyone who has had a rash, an itch or both within the past several weeks?
- Are you pregnant or nursing?
- Are you or is your child being treated or have you or your child recently been treated for any other medical conditions?
- What medications are you or your child taking, including prescription and nonprescription drugs, vitamins and supplements?
- Is your child in child care?
What you can do in the meantime
Before your appointment, try at-home and nonprescription remedies to help reduce itching. Allergy pills and calamine lotion may provide some relief. Ask your health care provider what nonprescription medications and lotions are safe for your child.
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


