Overview
Pancreatic cancer is a type of cancer that begins as a growth of cells in the pancreas. The pancreas lies behind the lower part of the stomach. It makes enzymes that help digest food and hormones that help manage blood sugar.
The most common type of pancreatic cancer is pancreatic ductal adenocarcinoma. This type begins in the cells that line the ducts that carry digestive enzymes out of the pancreas.
Pancreatic cancer rarely is found at its early stages when the chance of curing it is greatest. This is because it often doesn't cause symptoms until after it has spread to other organs.
Your health care team considers the extent of your pancreatic cancer when creating your treatment plan. Treatment options may include surgery, chemotherapy, radiation therapy or a mix of these.
Symptoms
Pancreatic cancer often doesn't cause symptoms until the disease is advanced. When they happen, signs and symptoms of pancreatic cancer may include:
- Belly pain that spreads to the sides or back.
- Loss of appetite.
- Weight loss.
- Yellowing of the skin and the whites of the eyes, called jaundice.
- Light-colored or floating stools.
- Dark-colored urine.
- Itching.
- New diagnosis of diabetes or diabetes that's getting harder to control.
- Pain and swelling in an arm or leg, which might be caused by a blood clot.
- Tiredness or weakness.
When to see a doctor
Make an appointment with a health care professional if you have symptoms that worry you.
Causes
It's not clear what causes pancreatic cancer. Doctors have found some factors that might raise the risk of this type of cancer. These include smoking and having a family history of pancreatic cancer.
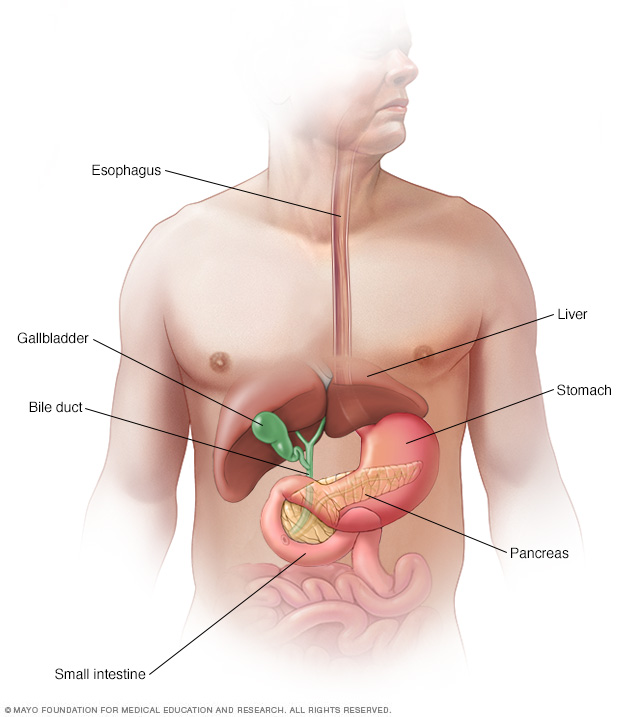
Understanding the pancreas
The pancreas is about 6 inches (15 centimeters) long and looks something like a pear lying on its side. It releases hormones, including insulin. These hormones help the body process the sugar in the foods you eat. The pancreas also makes digestive juices to help the body digest food and take in nutrients.
How pancreatic cancer forms
Pancreatic cancer happens when cells in the pancreas develop changes in their DNA. A cell's DNA holds the instructions that tell a cell what to do. In healthy cells, the instructions tell the cells to grow and multiply at a set rate. The cells die at a set time. In cancer cells, the changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes there to be too many cells.
The cancer cells might form a mass called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body.
Most pancreatic cancer begins in the cells that line the ducts of the pancreas. This type of cancer is called pancreatic ductal adenocarcinoma or pancreatic exocrine cancer. Less often, cancer can form in the hormone-producing cells or the neuroendocrine cells of the pancreas. These types of cancer are called pancreatic neuroendocrine tumors or pancreatic endocrine cancer.
Risk factors
Factors that might raise the risk of pancreatic cancer include:
- Smoking.
- Type 2 diabetes.
- Chronic inflammation of the pancreas, called pancreatitis.
- Family history of DNA changes that can increase cancer risk. These include changes in the BRCA2 gene, Lynch syndrome and familial atypical multiple mole melanoma (FAMMM) syndrome.
- Family history of pancreatic cancer.
- Obesity.
- Older age. Most people with pancreatic cancer are over 65.
- Drinking a lot of alcohol.
Complications
As pancreatic cancer progresses, it can cause complications such as:
- Weight loss. People with pancreatic cancer might lose weight as the cancer uses more of the body's energy. Nausea and vomiting caused by cancer treatments or a cancer pressing on the stomach might make it hard to eat. Sometimes the body has trouble getting nutrients from food because the pancreas isn't making enough digestive juices.
-
Jaundice. Pancreatic cancer that blocks the liver's bile duct can cause jaundice. Signs include yellowing of the skin and the whites of the eyes. Jaundice can cause dark-colored urine and pale-colored stools. Jaundice often occurs without belly pain.
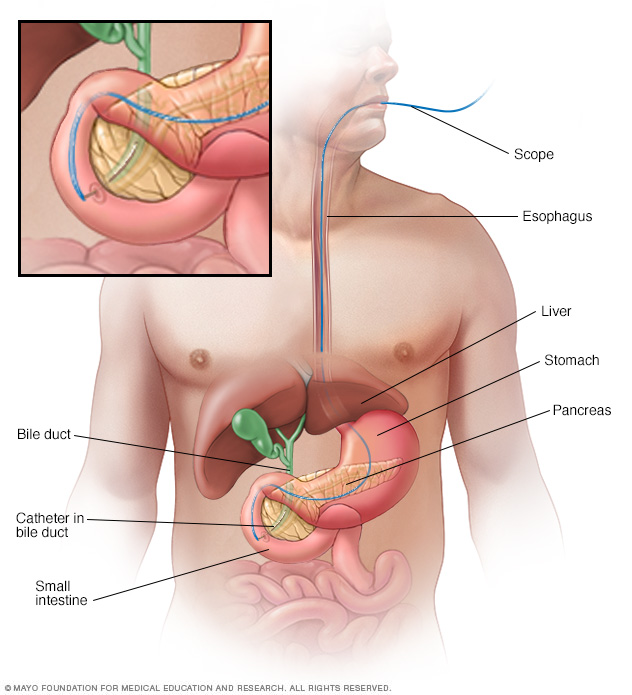
If the bile duct is blocked, a plastic or metal tube called a stent can be put inside it. The stent helps hold the bile duct open. This is done using a procedure called endoscopic retrograde cholangiopancreatography, also called ERCP.
During ERCP, a health care professional puts a long tube with a tiny camera, called an endoscope, down the throat. The tube goes through the stomach and into the upper part of the small intestine. The health professional puts a dye into the pancreatic ducts and bile ducts through a small tube that fits through the endoscope. The dye helps the ducts show up on imaging tests. The health professional uses those images to place a stent at the right spot in the duct to help hold it open.
-
Pain. A growing tumor may press on nerves in your abdomen, causing pain that can become severe. Pain medications can help you feel more comfortable. Treatments, such as radiation and chemotherapy, might help slow tumor growth and provide some pain relief.
When medicines aren't helping, a health care professional might suggest a celiac plexus block. This procedure uses a needle to put alcohol into the nerves that control pain in the belly. The alcohol stops the nerves from sending pain signals to the brain.
-
Bowel blockage. Pancreatic cancer can grow into or press on the first part of the small intestine, called the duodenum. This can block the flow of digested food from the stomach into the intestines.
A health care professional might suggest putting a tube called a stent in the small intestine to hold it open. Sometimes, it might help to have surgery to place a feeding tube. Or surgery can attach the stomach to a lower part of the intestines where the cancer isn't causing a blockage.
Prevention
Screening for people with a high risk of pancreatic cancer
Screening uses tests to look for signs of pancreatic cancer in people who don't have symptoms. It might be an option if you have a very high risk of pancreatic cancer. Your risk might be high if you have a strong family history of pancreatic cancer or if you have an inherited DNA change that increases the risk of cancer.
Pancreatic cancer screening might involve imaging tests, such as MRI and ultrasound. These tests are generally repeated every year.
The goal of screening is to find pancreatic cancer when it's small and most likely to be cured. Research is ongoing, so it's not yet clear whether screening can lower the risk of dying of pancreatic cancer. There are risks to screening. This includes the chance of finding something that requires surgery but later turns out to not be cancer.
Talk about the benefits and risks of pancreatic cancer screening with your health care team. Together you can decide whether screening is right for you.
Genetic testing for cancer risk
If you have a family history of pancreatic cancer, discuss it with a health care professional. The health professional can review your family history and help you understand whether genetic testing might be right for you.
Genetic testing can find DNA changes that run in families and increase the risk of cancer. If you're interested in genetic testing, you might be referred to a genetic counselor or other health care professional trained in genetics.
Ways to lower risk
You might reduce your risk of pancreatic cancer if you:
- Stop smoking. If you smoke, talk to a member of your health care team about ways to help you stop. These might include support groups, medicines and nicotine replacement therapy.
- Maintain a healthy weight. If you are at a healthy weight, work to maintain it. If you need to lose weight, aim for a slow, steady weight loss of 1 to 2 pounds (0.5 to 1 kilogram) a week. To help you lose weight, exercise most days of the week. Slowly increase the amount of exercise you get. Choose a diet rich in vegetables, fruit and whole grains with smaller portions.
Diagnosis
Tests used to diagnose pancreatic cancer include:
- Imaging tests. Imaging tests take pictures that show the inside of the body. Imaging tests used to diagnose pancreatic cancer include ultrasound, CT scans, MRI scans and, sometimes, positron emission tomography scans, also called PET scans.
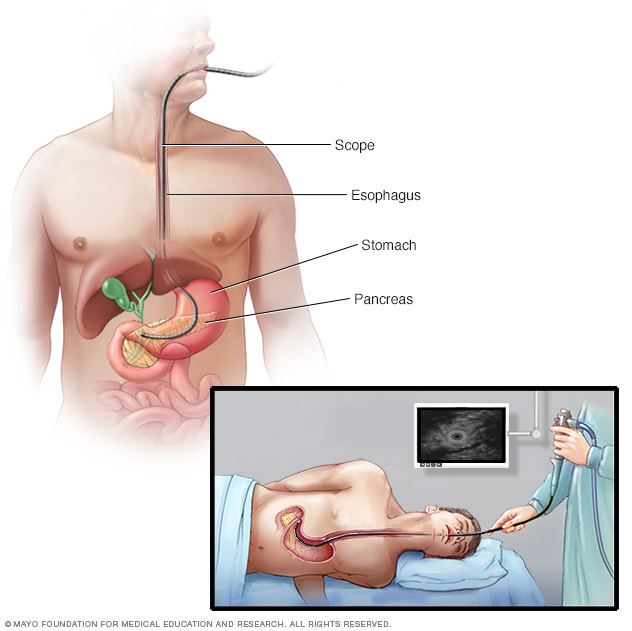
- A scope with ultrasound. Endoscopic ultrasound, also called EUS, is a test to make pictures of the digestive tract and nearby organs and tissues. EUS uses a long, thin tube with a camera, called an endoscope. The endoscope passes down the throat and into the stomach. An ultrasound device on the endoscope uses sound waves to create images of nearby tissues. It can be used to make pictures of the pancreas.
Removing a tissue sample for testing. A biopsy is a procedure to remove a small sample of tissue for testing in a lab. Most often, a health professional gets the sample during EUS. During EUS, special tools are passed through the endoscope to take some tissue from the pancreas. Less often, a sample of tissue is collected from the pancreas by inserting a needle through the skin and into the pancreas. This is called fine-needle aspiration.
The sample goes to the lab for testing to see if its cancer. Other specialized tests can show what DNA changes are present in the cancer cells. The results help your health care team create your treatment plan.
- Blood tests. Blood tests might show proteins called tumor markers that pancreatic cancer cells make. One tumor marker test used in pancreatic cancer is called CA19-9. Doctors often repeat this test during and after treatment to understand how the cancer is responding. Some pancreatic cancers don't make extra CA19-9, so this test isn't helpful for everyone.
- Genetic testing. If you're diagnosed with pancreatic cancer, talk with your health care team about genetic testing. Genetic testing uses a sample of blood or saliva to look for inherited DNA changes that increase the risk of cancer. Results of genetic testing might help guide your treatment. The results also can show whether family members might have an increased risk of pancreatic cancer.
Staging
After confirming a diagnosis of pancreatic cancer, your health care team works to find the extent of the cancer. This is called the stage of the cancer. Your health care team uses your cancer's stage to understand your prognosis and create a treatment plan.
The stages of pancreatic cancer use the numbers 0 to 4. In the lowest stages, the cancer is only in the pancreas. As the cancer grows, the stage increases. By stage 4, the cancer has spread to other parts of the body.
Treatment
Treatment for pancreatic cancer depends on the stage of the cancer and the location. Your health care team also considers your overall health and your preferences. For most people, the first goal of pancreatic cancer treatment is to get rid of the cancer, when possible. When that isn't possible, the focus may be on improving quality of life and keeping the cancer from growing or causing more harm.
Pancreatic cancer treatments may include surgery, radiation, chemotherapy or a combination of these. When the cancer is advanced, these treatments aren't likely to help. So treatment focuses on relieving symptoms to keep you as comfortable as possible for as long as possible.
Surgery
Surgery can cure pancreatic cancer, but it's not an option for everyone. It might be used to treat cancer that hasn't spread to other organs. Surgery might not be possible if the cancer grows large or extends into nearby blood vessels. In these situations, treatment might start with other options, such as chemotherapy. Sometimes surgery might be done after these other treatments.
Operations used to treat pancreatic cancer include:
-
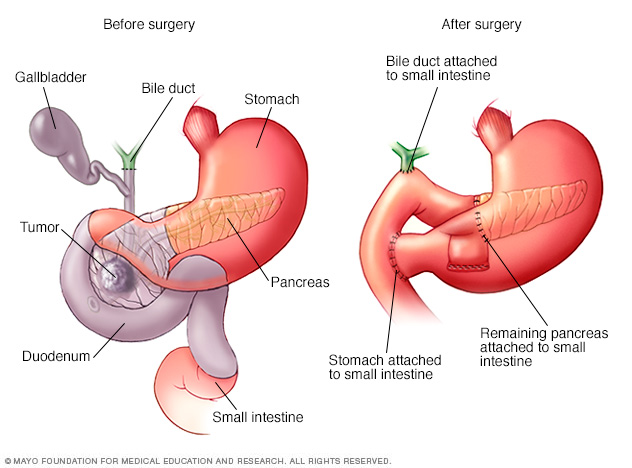
Surgery for cancers in the pancreatic head. The Whipple procedure, also called pancreaticoduodenectomy, is an operation to remove the head of the pancreas. It also involves removing the first part of the small intestine and the bile duct. Sometimes the surgeon removes part of the stomach and nearby lymph nodes. The remaining organs are rejoined to allow food to move through the digestive system.
- Surgery for cancers in the body and tail of the pancreas. Surgery to remove the body and tail of the pancreas is called distal pancreatectomy. With this procedure, the surgeon also might need to remove the spleen.
- Surgery to remove the whole pancreas. This is called total pancreatectomy. After surgery, you'll take medicine to replace the hormones and enzymes made by the pancreas for the rest of your life.
- Surgery for cancers that affect nearby blood vessels. When a cancer in the pancreas grows to involve nearby blood vessels, a more-complex procedure might be needed. The procedure might need to involve taking out and rebuilding parts of the blood vessels. Few medical centers in the United States have surgeons trained to do these blood vessel operations safely.
Each of these operations carries the risk of bleeding and infection. After surgery some people have nausea and vomiting if the stomach has trouble emptying, called delayed gastric emptying. Expect a long recovery after any of these procedures. You'll spend several days in the hospital and then recover for several weeks at home.
Research shows that pancreatic cancer surgery tends to cause fewer complications when done by highly experienced surgeons at centers that do many of these operations. Ask about your surgeon's and hospital's experience with pancreatic cancer surgery. If you have any doubts, get a second opinion.
Chemotherapy
Chemotherapy uses strong medicines to kill cancer cells. Treatment might involve one chemotherapy medicine or a mix of them. Most chemotherapy medicines are given through a vein, but some are taken in pill form.
Chemotherapy might be the first treatment used when the first treatment can't be surgery. Chemotherapy also might be given at the same time as radiation therapy. Sometimes this combination of treatments shrinks the cancer enough to make surgery possible. This approach to treatment is offered at specialized medical centers that have experience caring for many people with pancreatic cancer.
Chemotherapy is often used after surgery to kill any cancer cells that might remain.
When the cancer is advanced and spreads to other parts of the body, chemotherapy can help control it. Chemotherapy might help relieve symptoms, such as pain.
Radiation therapy
Radiation therapy uses powerful energy beams to kill cancer cells. The energy can come from X-rays, protons or other sources. During radiation therapy, you lie on a table while a machine moves around you. The machine directs radiation to precise points on your body.
Radiation can be used either before or after surgery. It's often done after chemotherapy. Radiation also can be combined with chemotherapy.
When surgery isn't an option, radiation therapy and chemotherapy might be the first treatment. This combination of treatments might shrink the cancer and make surgery possible.
When the cancer spreads to other parts of the body, radiation therapy can help relieve symptoms, such as pain.
Immunotherapy
Immunotherapy is a treatment with medicine that helps the body's immune system kill cancer cells. The immune system fights off diseases by attacking germs and other cells that shouldn't be in the body. Cancer cells survive by hiding from the immune system. Immunotherapy helps the immune system cells find and kill the cancer cells. Immunotherapy might be an option if your pancreatic cancer has specific DNA changes that would make the cancer likely to respond to these treatments.
Clinical trials
Clinical trials are studies of new treatments. These studies provide a chance to try the latest treatments. The risk of side effects might not be known. Ask your health care professional if you might be able to be in a clinical trial.
Palliative care
Palliative care is a special type of health care that helps people with serious illness feel better. If you have cancer, palliative care can help relieve pain and other symptoms. A team of health care professionals does palliative care. The team can include doctors, nurses and other specially trained professionals. The team's goal is to improve quality of life for you and your family.
Palliative care specialists work with you, your family and your care team to help you feel better. They provide an extra layer of support while you have cancer treatment. You can have palliative care at the same time as strong cancer treatments, such as surgery, chemotherapy or radiation therapy.
When palliative care is used with all the other appropriate treatments, people with cancer may feel better and live longer.
Alternative medicine
Some integrative medicine and alternative therapies may help with symptoms caused by cancer or cancer treatments.
Treatments to help you cope with distress
People with cancer often have distress. Distress might feel like worry, fear, anger and sadness. If have these feelings, you may find it hard to sleep. You might think about your cancer all the time.
Discuss your feelings with a member of your health care team. Specialists can help you sort through your feelings. They can help you find ways to cope. In some cases, medicines may help.
Integrative medicine and alternative therapies also may help you cope with your feelings. Examples include:
- Art therapy.
- Exercise.
- Meditation.
- Music therapy.
- Relaxation exercises.
- Spirituality.
Talk with a member of your health care team if you'd like to try some of these treatment options.
Coping and support
Learning you have a life-threatening illness can feel stressful. Some of the following suggestions may help:
-
Learn about your cancer. Learn enough about your cancer to help you make decisions about your care. Ask a member of your health care team about the details of your cancer and your treatment options. Ask about trusted sources of more information.
If you're doing your own research, good places to start are the National Cancer Institute and the Pancreatic Cancer Action Network.
- Put together a support system. Ask your friends and family to form a support network for you. They might not know what to do after your diagnosis. Helping you with simple tasks might give them comfort and relieve you of those tasks. Think of things you want help with, such as making meals or getting to appointments.
- Find someone to talk with. Although friends and family can often be your best support, sometimes they might find it hard to cope with your diagnosis. It might help to talk with a counselor, medical social worker, or a pastoral or religious counselor. Ask a member of your health care team for a referral.
- Connect with other cancer survivors. You may find comfort in talking with other cancer survivors. Contact your local chapter of the American Cancer Society to find cancer support groups in your area. The Pancreatic Cancer Action Network offers support groups online and in person.
- Consider hospice. Hospice care provides comfort and support to people at the end of life and their loved ones. It allows family and friends, with the aid of nurses, social workers and trained volunteers, to care for and comfort a loved one at home or in a hospice setting. Hospice care also gives emotional, social and spiritual support for people who are ill and those closest to them.
Preparing for an appointment
Start by making an appointment with a doctor or other health care professional if you have symptoms that worry you. You might then be referred to:
- A doctor who diagnoses and treats digestive conditions, called a gastroenterologist.
- A doctor who treats cancer, called an oncologist.
- A doctor who uses radiation to treat cancer, called a radiation oncologist.
- A surgeon who specializes in operations on the pancreas, called a surgical oncologist.
What you can do
When you call to make the appointment, ask about anything you need to do for the appointment, such as restricting your diet. Ask a relative or friend to go with you to help you remember all the information.
Make a list of:
- All your symptoms and when they began.
- Key personal information, including any recent changes or stressors and family history of pancreatic cancer.
- All your medicines, vitamins and supplements, including doses.
Questions to ask your doctor
- Do I have pancreatic cancer?
- What is the stage of my cancer?
- Will I need more tests?
- Can my cancer be cured?
- What are my treatment options?
- Can any treatment help me live longer?
- What are the potential risks of each treatment?
- Is there one treatment you think is best for me?
- What advice would you give a friend or a family member in my situation?
- What is your experience with pancreatic cancer diagnosis and treatment? How many surgical procedures for this type of cancer does this medical center do each year?
- What can be done to help ease my symptoms?
- What clinical trials are available for pancreatic cancer? Am I eligible for any?
- Am I eligible for molecular profiling of my cancer?
- Do you have brochures or other printed material that I can take? What websites do you recommend?
What to expect from your doctor
Be prepared to answer some questions about your symptoms and your health, such as:
- Do you have symptoms all the time, or do they come and go?
- Do your symptoms get in the way of your everyday activities?
- Does anything make your symptoms worse or better?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


