Overview
A molar pregnancy is a rare complication of pregnancy. It involves unusual growth of cells called trophoblasts. These cells typically become the organ that feeds a growing fetus. That organ also is known as the placenta.
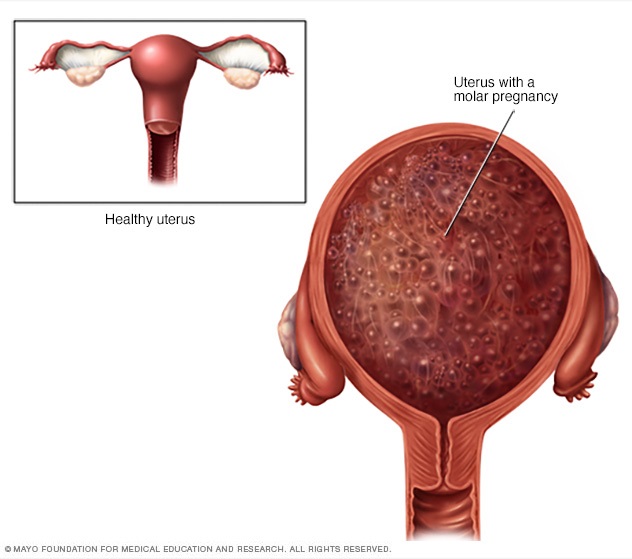
There are two types of molar pregnancy — complete molar pregnancy and partial molar pregnancy. In a complete molar pregnancy, the placental tissue swells and appears to form fluid-filled cysts. There is no fetus.
In a partial molar pregnancy, the placenta might have both regular and irregular tissue. There may be a fetus, but the fetus can't survive. The fetus usually is miscarried early in the pregnancy.
A molar pregnancy can have serious complications, including a rare form of cancer. A molar pregnancy requires early treatment.
Symptoms
A molar pregnancy may seem like a regular pregnancy at first. But most molar pregnancies cause symptoms that can include:
- Dark brown to bright red bleeding from the vagina during the first three months
- Severe nausea and vomiting
- Sometimes grapelike cysts that pass from the vagina
- Pelvic pressure or pain
Because of improved ways of detecting a molar pregnancy, most are found in the first trimester. If it is not found in the first three months, symptoms of a molar pregnancy might include:
- A uterus growing quickly and being too large early in the pregnancy
- Preeclampsia — a condition that causes high blood pressure and protein in the urine — before 20 weeks of pregnancy
- Ovarian cysts
- Overactive thyroid, also known as hyperthyroidism
Causes
An egg fertilized atypically causes a molar pregnancy. Human cells usually have 23 pairs of chromosomes. In a typical fertilization, one chromosome in each pair comes from the father, the other from the mother.
In a complete molar pregnancy, one or two sperm fertilize an egg. The chromosomes from the mother's egg are missing or don't work. The father's chromosomes are copied. There's none from the mother.
In a partial or incomplete molar pregnancy, the mother's chromosomes are present, but the father supplies two sets of chromosomes. The embryo then has 69 chromosomes instead of 46. This most often occurs when two sperm fertilize an egg, resulting in an extra copy of the father's genes.
Risk factors
Factors that can contribute to a molar pregnancy include:
- Earlier molar pregnancy. If you've had one molar pregnancy, you're more likely to have another. A repeat molar pregnancy happens, on average, in 1 out of every 100 people.
- Age of the mother. A molar pregnancy is more likely in people older than age 43 or younger than age 15.
Complications
After removing a molar pregnancy, molar tissue might remain and continue to grow. This is called persistent gestational trophoblastic neoplasia (GTN). GTN happens more often in complete molar pregnancies than it does in partial molar pregnancies.
One sign of persistent GTN is a high level of human chorionic gonadotropin (HCG) — a pregnancy hormone — after the molar pregnancy has been removed. In some cases, the mole that causes the molar pregnancy goes deep into the middle layer of the uterine wall. This causes bleeding from the vagina.
Persistent GTN is usually treated with chemotherapy. Another treatment possibility is removal of the uterus, also known as hysterectomy.
Rarely, a cancerous form of GTN known as choriocarcinoma develops and spreads to other organs. Choriocarcinoma is usually successfully treated with chemotherapy. A complete molar pregnancy is more likely to have this complication than is a partial molar pregnancy.
Prevention
If you've had a molar pregnancy, talk to your pregnancy care provider before trying to get pregnant again. You might want to wait six months to one year. The risk of having another molar pregnancy is low, but it's higher once you've had a molar pregnancy.
During future pregnancies, a care provider may do early ultrasounds to check your condition and make sure the baby is developing.
Diagnosis
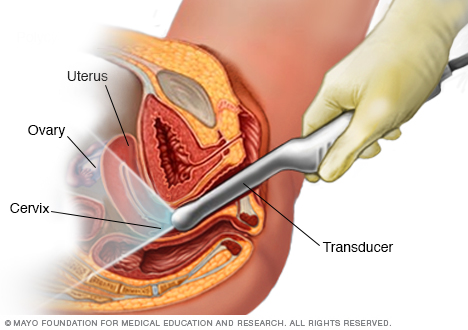
A health care provider who suspects a molar pregnancy is likely to order blood tests and an ultrasound. During early pregnancy, a sonogram might involve a wandlike device placed in the vagina.
As early as eight or nine weeks of pregnancy, an ultrasound of a complete molar pregnancy might show:
- No embryo or fetus
- No amniotic fluid
- A thick cystic placenta nearly filling the uterus
- Ovarian cysts
An ultrasound of a partial molar pregnancy might show:
- A fetus that's smaller than expected
- Low amniotic fluid
- Placenta that appears unusual
After finding a molar pregnancy, a health care provider might check for other medical issues, including:
- Preeclampsia
- Hyperthyroidism
- Anemia
Treatment
A molar pregnancy can't be allowed to continue. To prevent complications, the affected placental tissue must be removed. Treatment usually consists of one or more of the following steps:
-
Dilation and curettage (D&C). This procedure removes the molar tissue from the uterus. You lie on a table on your back with your legs in stirrups. You receive medicine to numb you or put you to sleep.
After opening the cervix, the provider removes uterine tissue with a suction device. A D&C for a molar pregnancy usually is done in a hospital or surgery center.
- Removal of the uterus. This occurs rarely if there's increased risk of gestational trophoblastic neoplasia (GTN) and there's no desire for future pregnancies.
-
HCG monitoring. After the molar tissue is removed, a provider keeps measuring the HCG level until it goes down. A continuing high level of HCG in the blood might require more treatment.
After treatment for the molar pregnancy is complete, a provider might check HCG levels for six months to make sure no molar tissue is left. For people with GTN, HCG levels are checked for one year after chemotherapy is completed.
Because pregnancy HCG levels also increase during a regular pregnancy, a provider might recommend waiting 6 to 12 months before trying to become pregnant again. The provider can recommend a reliable form of birth control during this time.
Coping and support
Losing a pregnancy can be very hard. Give yourself time to grieve. Talk about your feelings and allow yourself to feel them fully. Turn to your partner, family or friends for support. If you're having trouble handling your emotions, talk to your pregnancy care provider or a counselor.
Preparing for an appointment
You're likely to start by seeing your family care provider or pregnancy care provider. Here's some information to help you get ready for your appointment.
What you can do
Ask a friend or family member to go with you to your appointment, if possible. Having someone there may help you remember the information you get. Make a list of the following:
- Your symptoms, including when they started and how they've changed over time.
- The date of your last menstrual period, if you remember it.
- Key personal information, including other medical conditions you have.
- All medications, vitamins or supplements you take, including doses.
- Questions to ask your provider.
For molar pregnancy, some questions to ask include:
- What is likely causing my symptoms?
- What tests do I need?
- What treatment do you recommend?
- Do I need to follow any restrictions?
- What emergency symptoms should I watch for at home?
- What are my chances of giving birth in the future?
- How long should I wait before trying to become pregnant again?
- Does my condition increase my risk of developing cancer in the future?
- Do you have brochures or printed material that I can have? What websites do you recommend?
Don't hesitate to ask other questions you have.
What to expect from your doctor
Your health care provider might ask you questions, such as:
- Have your symptoms been ongoing or occasional?
- Are you having pain?
- Compared with your heaviest days of menstrual flow, is your bleeding more, less or about the same? Have you passed grapelike cysts from your vagina?
- Have you been lightheaded or dizzy?
- Have you had a past molar pregnancy?
- Do you wish to become pregnant in the future?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


