Overview
Lichen sclerosus (LIE-kun skluh-ROW-sus) is a condition that causes patchy, discolored, thin skin. It usually affects the genital and anal areas.
Anyone can get lichen sclerosus but postmenopausal women are at higher risk. It isn't contagious and can't be spread through sexual contact.
Treatment is usually a medicated ointment. This treatment helps return the skin to its usual color and reduces the risk of scarring. Even if your symptoms clear up, they tend to come back. So you'll likely need long-term follow-up care.
Symptoms
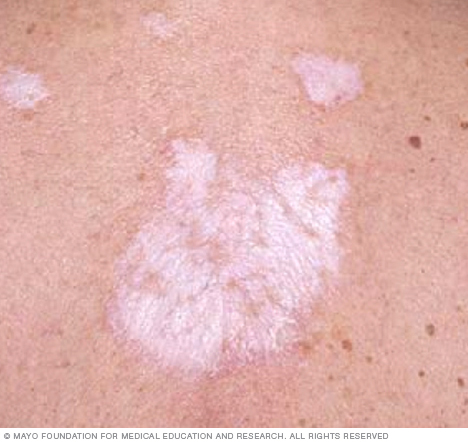
It's possible to have mild lichen sclerosus with no symptoms. When symptoms do occur, they usually affect the skin of the genital and anal areas. The back, shoulders, upper arms and breasts may also be affected. Symptoms may include:
- Smooth discolored skin patches
- Blotchy, wrinkled skin patches
- Itching
- Soreness or a burning feeling
- Easy bruising
- Fragile skin
- Changes in the tube for urine flow (urethra)
- Bleeding, blistering or open sores
- Painful sex
When to see a doctor
See your health care provider if you have symptoms of lichen sclerosus.
If you've already been diagnosed with lichen sclerosus, see your health care provider every 6 to 12 months. These visits are important to check for any skin changes or side effects of treatment.
Causes
The exact cause of lichen sclerosus isn't known. It's likely a combination of factors, including an overactive immune system, your genetic makeup, and previous skin damage or irritation.
Lichen sclerosus isn't contagious and can't be spread through sexual contact.
Risk factors
Anyone can get lichen sclerosus, but the risk is higher for:
- Postmenopausal women
- Children younger than 10 years old
- Women who have another autoimmune disease, such as forms of low thyroid function (hypothyroidism)
- Men with urinary incontinence or an uncircumcised penis
- People with a family history of the disease
Complications
Complications of lichen sclerosus include painful sex and scarring, including covering of the clitoris. Scarring of the penis can cause painful erection, poor urine flow and an inability to retract the foreskin.
People with vulvar lichen sclerosus are also at an increased risk of squamous cell carcinoma.
In children, constipation is a common complication.
Diagnosis
Your health care provider may diagnose lichen sclerosus by looking at the affected skin. You may need a biopsy to rule out cancer. You may need a biopsy if your skin doesn't respond to steroid creams. A biopsy involves removing a small piece of affected tissue for examination under a microscope.
You may be referred to specialists in skin conditions (dermatologist), the female reproductive system (gynecologist), urology and pain medicine.
Treatment
With treatment, symptoms often improve or go away. Treatment for lichen sclerosus depends on how severe your symptoms are and where it is on your body. Treatment can help ease itching, improve how your skin looks and decrease the risk of scarring. Even with successful treatment, the symptoms often come back.
Medicated ointments
Steroid ointment clobetasol is commonly prescribed for lichen sclerosus. At first you'll need to apply the ointment to the affected skin twice a day. After several weeks, your health care provider will likely suggest that you use it only twice a week to prevent symptoms from returning.
Your health care provider will monitor you for side effects associated with prolonged use of topical corticosteroids, such as further thinning of the skin.
In addition, your health care provider may recommend a calcineurin inhibitor, such as tacrolimus ointment (Protopic).
Ask your health care provider how often you'll need to return for follow-up exams — likely once or twice a year. Long-term treatment is needed to control itching and irritation and prevent serious complications.
Circumcision
Your health care provider might recommend removing the penis foreskin (circumcision) if the opening for urine flow has been narrowed by lichen sclerosus.
Lifestyle and home remedies
These self-care tips may help ease skin irritation:
- Apply petroleum jelly (Vaseline, Aquaphor, others) to the affected area.
- Gently wash the affected area daily and pat dry. Use mild unscented soaps and avoid bathing too much.
- Ease burning and pain with a bath in the morning and at night, with water that's comfortable to the touch. Don't add bubble bath or other products.
- Take an oral antihistamine at bedtime to help control the itching as you try to sleep.
- Use soft unscented toilet paper without dyes.
- Avoid irritants, such as tight clothing and scented detergents.
Preparing for an appointment
If you have symptoms of lichen sclerosus, make an appointment with your health care provider. You may be referred to a specialist in the diagnosis and treatment of skin conditions (dermatologist).
Here's some information to help you get ready for your appointment.
What you can do
Before your appointment make a list of:
- Your symptoms and how long you've had them.
- Your key medical information, such as other conditions with which you've been diagnosed and any prescription or over-the-counter medications you're using, including vitamins and supplements.
- Questions to ask your health care provider.
Some basic questions to ask your health care provider about possible lichen sclerosus include:
- What's the most likely cause of my symptoms?
- What treatment approach do you suggest, if any?
- If the first treatment doesn't work, what will you suggest next?
- How much do you expect my symptoms will improve with treatment — and how soon?
- Will I need treatment for this condition for the rest of my life?
- What self-care steps can I follow to ease my symptoms?
- What can I do to help prevent the symptoms from coming back?
What to expect from your doctor
Your health care provider is likely to ask you questions, such as:
- How severe is your discomfort?
- Have you noticed any bleeding?
- Do your symptoms include pain with urination or bowel movements?
- Do your symptoms include pain with sexual intercourse?
- Have you had any previous injuries to the affected area?
- What steps have you taken to treat this condition yourself?
- Have you had prescription treatments for this condition?
- Have you been diagnosed with any other medical conditions?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


