Overview
Immune thrombocytopenia (ITP) is an illness that can lead to bruising and bleeding. Low levels of the cells that help blood clot, also known as platelets, most often cause the bleeding.
Once known as idiopathic thrombocytopenic purpura, ITP can cause purple bruises. It also can cause tiny reddish-purple dots on the skin that look like a rash.
Children can get ITP after a virus. They most often get better without treatment. In adults, the illness often lasts months or years.
People with ITP who aren't bleeding and whose platelet count isn't too low might not need treatment. For worse symptoms, treatment might include medicines to raise platelet count or surgery to remove the spleen.
Symptoms
Immune thrombocytopenia might not have symptoms. When symptoms occur, they might include:
- Easy bruising.
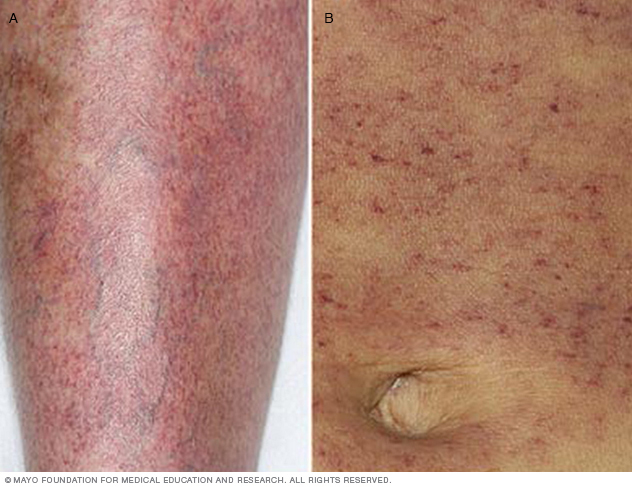
- Bleeding into the skin that looks like tiny reddish-purple spots, also known as petechiae. The spots mostly show up on the lower legs. They look like a rash.
- Bleeding into the skin that's larger than petechiae, also known as purpura.
- Bleeding from the gums or nose.
- Blood in urine or stools.
- Really heavy menstrual flow.
When to see a doctor
Make an appointment with your health care provider if you or your child has symptoms that worry you. Bleeding that won't stop is a medical emergency. Seek help right away if you or your child has bleeding that the usual first aid efforts can't control. These include applying pressure to the area.
Causes
Immune thrombocytopenia usually happens when the immune system makes a mistake. It attacks and destroys the cells that help blood clot, also known as platelets.
In adults, an infection with HIV, hepatitis or the bacteria that causes stomach ulcers, known as H. pylori, can cause ITP. In most children with ITP, the disorder follows a virus, such as the mumps or the flu.
Risk factors
ITP is more common among young women. The risk appears to be higher in people who also have other diseases in which the immune system attacks healthy tissues, such as rheumatoid arthritis or lupus.
Complications
Rarely, immune thrombocytopenia causes bleeding into the brain. This can be fatal.
Someone who's pregnant with a low platelet count or who's bleeding has a greater risk of heavy bleeding during delivery. A health care provider might suggest treatment to keep the platelet count even.
ITP doesn't usually affect the fetus. However, the baby's platelet count should be tested soon after birth.
Diagnosis
To diagnose immune thrombocytopenia, a health care provider will try to rule out other possible causes of bleeding and a low platelet count.
No one test can prove the diagnosis. Blood tests can check platelet levels. Rarely, adults might need a bone marrow biopsy to rule out other problems.
Treatment
People with mild immune thrombocytopenia might need only regular platelet checks. Children usually improve without treatment. Most adults with ITP will need treatment at some point. The condition often gets worse or lasts long, also known as chronic.
Treatment might include medicines to increase platelet count or surgery to remove the spleen, known as a splenectomy. A health care provider can talk about the pros and cons of treatment options. Some people find the side effects of treatment are worse than the disease.
Medications
Make sure your health care provider knows about medicines or supplements you take without a prescription. You might need to stop using any that might increase bleeding. Examples include aspirin, ibuprofen (Advil, Motrin IB, others) and ginkgo biloba.
Medicines to treat ITP may include:
- Steroids. Health care providers often use an oral corticosteroid, such as prednisone. When the platelet count is back to a safe level, the provider can tell how to cut down the medicine a little at a time. Long-term use of these medicines can increase the risk of infections, high blood sugar and osteoporosis.
- Immune globulin. If corticosteroids don't work, a shot of immune globulin might help. This medicine also treats serious bleeding or quickly increases blood count before surgery. The effect usually wears off in a couple of weeks.
- Drugs that increase platelets. Medicines such as romiplostim (Nplate), eltrombopag (Promacta) and avatrombopag (Doptelet) help bone marrow make more platelets. These types of medicines can increase the risk of blood clots.
-
Other drugs. Rituximab (Rituxan, Ruxience, Truxima) helps increase the platelet count by reducing the immune system response damaging them. But this medicine also can keep vaccinations from working well. Later surgery to remove the spleen might increase the need for the protection against illness that vaccinations give.
Fostamatinib (Tavalisse) is a newer drug approved for people with long-lasting ITP who haven't responded to other treatments.
Surgery
If medicine doesn't make ITP better, surgery to remove the spleen might be the next step. When it works, this surgery quickly ends the attacks on platelets and improves platelet count.
But taking out the spleen doesn't work for everyone. And not having a spleen increases the risk of infection.
Emergency treatment
Rarely, ITP can cause a lot of bleeding. Emergency care usually includes getting blood, also known as transfusion, that contains many platelets. Steroids and immune globulin given through a tube in a vein also might help.
Lifestyle and home remedies
If you have immune thrombocytopenia, try to:
- Avoid contact sports. Getting hit in the head during sports like boxing, martial arts and football could cause bleeding in the brain. Talk to your health care provider about what activities are safe.
- Watch for signs of infection. If you've had your spleen removed, look for signs of infection, including fever. Get treatment quickly. Infections can be worse in people without spleens.
- Take care with medicines you get without a prescription. Medicines such as aspirin and ibuprofen (Advil, Motrin IB, others) can increase bleeding risk.
Preparing for an appointment
A low platelet count might not cause symptoms so a blood test for something else often finds the problem.
Diagnosing immune thrombocytopenia usually involves more blood tests. Your provider might send you to a specialist in blood diseases, also known as a hematologist.
What you can do
Here are some steps to take to get ready for your appointment. Taking a family member or friend with you can help you remember the information you get.
Make a list of:
- Your symptoms and when they began. Include symptoms that don't seem to be linked to the reason you made the appointment.
- Key personal information, including major stresses, life changes, and recent illnesses or medical procedures, such as receiving blood.
- All medicines, vitamins and other supplements you take, including doses.
- Questions to ask your provider.
Questions about ITP might include:
- How many platelets do I have in my blood?
- Is my platelet count too low?
- What is causing my ITP?
- Do I need more tests?
- Is this condition temporary or long lasting?
- What treatments are there? What do you recommend?
- What are the possible side effects of these treatments?
- What will happen if I do nothing?
- Are there any restrictions that I need to follow?
- Do you have brochures or other printed material that I can take? What websites do you recommend?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


