Overview
Hypospadias (hi-poe-SPAY-dee-us) is a condition that happens as the unborn baby, called a fetus, develops in the womb. The opening of the urethra is on the underside of the penis instead of at the tip. The urethra is the tube that drains urine from the bladder and out of the body.
Hypospadias is common and doesn't cause difficulty in caring for your baby. Surgery usually can create a typical looking penis that works properly. With successful treatment of hypospadias, most men can pass urine properly. And with successful hypospadias treatment, the condition won't block sperm from fertilizing an egg.
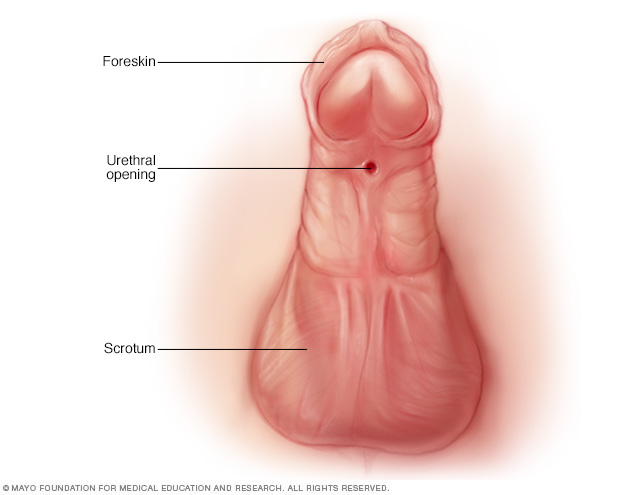
Symptoms
In hypospadias, the opening of the urethra is on the underside of the penis instead of at the tip. In most cases, the opening of the urethra is within the head of the penis. Less often, the opening is at the middle or the base of the penis. Rarely, the opening is in or beneath the scrotum.
Symptoms of hypospadias may include:
- Opening of the urethra at a place other than the tip of the penis.
- Downward curve of the penis. This condition is called chordee.
- Hooded appearance of the penis because only the top half of the penis is covered by foreskin.
- Differences in spraying when passing urine.
When to see a doctor
Most babies with hypospadias are diagnosed soon after birth while still in the hospital. But it may be harder to identify hypospadias if there's only a slight change in where the urethral opening is. Talk with your doctor or other healthcare professional if you have concerns about the look of your child's penis or if your child has problems passing urine.
Causes
Hypospadias is a condition that is present at birth. As the penis develops in a male unborn baby, certain hormones stimulate how the urethra and foreskin form. Hypospadias results from a change in the action of these hormones. This keeps the two sides of the urethral folds from joining completely. The location of the urethral opening depends on when the joining stopped.
In most cases, the exact cause of hypospadias is not known. Sometimes, hypospadias is caused by gene changes, but environment also may play a role.
Risk factors
Although the cause of hypospadias is usually not known, these factors may be linked with the condition:
- Family history. This condition is more common in babies with a family history of hypospadias.
- Genetics. Some gene changes may play a role in changing the hormones that stimulate how the male genitals develop.
- Maternal age over 35. Some research suggests that there may be a higher risk of hypospadias in male babies born to women older than 35 years.
- Exposure to certain substances during pregnancy. A link between hypospadias and a mother's exposure to certain hormones or certain compounds such as pesticides or industrial chemicals is being looked at. But more research is needed to confirm this link.
Complications
If hypospadias is not treated, it can result in:
- Differences in how the penis looks.
- Problems learning to use a toilet.
- Unusual curve of the penis with an erection.
- Problems releasing sperm from the penis. This release is called an ejaculation.
Diagnosis
Your child's pediatrician can diagnose hypospadias based on a physical exam. You'll likely be referred to a surgeon who specializes in genital and urinary conditions, called a pediatric urologist, for more evaluation. Medical centers with specialty teams can help you look at treatment options and can provide expert treatment.
When the opening of the urethra is not at the tip of the penis and the testicles can't be felt on exam, the genitals may be hard to identify as clearly male or female. This is called atypical genitalia. When this happens, more evaluation by a multispecialty team is recommended.
Treatment
Some forms of hypospadias are very minor and do not need surgery. But treatment usually involves surgery to put the urethral opening at the tip of the penis. If needed, surgery to straighten the shaft of the penis also is done. Surgery usually takes place between the ages of 6 and 12 months.
Circumcision likely won't be done if the penis looks different from usual. Instead, the foreskin tissue may be left in place for use during surgery to create a penis that looks and works properly. If hypospadias is found during circumcision, the procedure is usually finished. In either situation, referral to a pediatric urologist is recommended.
Surgery
For most forms of hypospadias, treatment involves a single surgery that's done on an outpatient basis. Some forms of hypospadias require more than one surgery.
When the urethral opening is near the base of the penis, the surgeon may need to use tissue grafts from the foreskin or from the inside of the mouth to reconstruct the urinary channel in the proper position.
Results of surgery
For most men, surgery is highly successful. Most of the time the penis looks typical after surgery. Most men can pass urine properly. And with successful hypospadias treatment, the condition won't block sperm from fertilizing an egg.
Occasionally, a hole called a fistula develops along the underside of the penis where the new urinary channel was created. This results in urine leaking. Rarely, there is a problem with wound healing or scarring. These complications may need another surgery for repair.
Follow-up care
Your child will need a couple of visits to the surgeon after surgery. After that, regular follow-up with your child's pediatric urologist is recommended after toilet training and at puberty to check for healing and possible complications.
Preparing for an appointment
Most often, babies with hypospadias are diagnosed while still in the hospital after birth. If your baby has hypospadias, you'll likely be referred to a pediatric urologist. Here's some information to help you get ready for your appointment.
What you can do
Before the appointment:
- Ask a family member or friend to go with you — that person can help you remember information and provide support.
- Make a list of questions to ask your doctor or other healthcare professional.
Questions to ask might include:
- Does my child need to have surgery?
- When is the best time for surgery?
- What are the risks with this surgery?
- What happens if my child doesn't have the surgery?
- Will this condition affect my child's fertility or sexual function later in life?
- What is the likelihood of future children having the same condition?
- Are there any brochures or other printed material that I can have?
- What websites do you suggest?
Feel free to ask other questions during the appointment.
What to expect from your doctor
Be ready to answer questions from your baby's healthcare professional, such as:
- Has anyone else in your family been diagnosed with hypospadias?
- Does your child's penis curve downward during an erection?
- Have you noticed any unusual spraying when your child passes urine?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


