Overview
Hypopituitarism is a rare condition in which the pituitary gland doesn't make one or more hormones or doesn't make enough hormones.
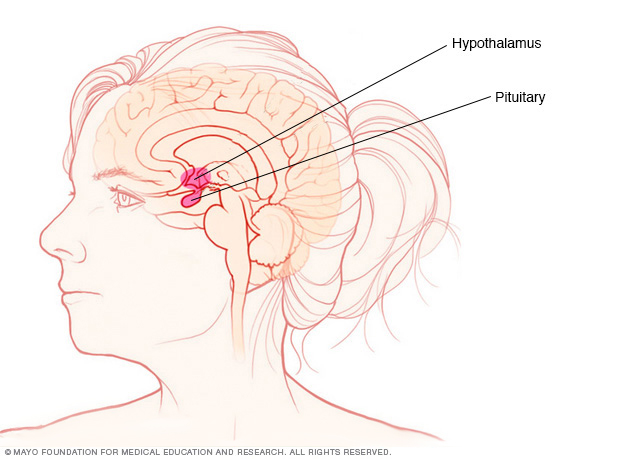
The pituitary gland is a kidney-bean-sized gland at the base of your brain. It is part of the body's system of glands that make hormones, called the endocrine system. The pituitary gland makes several hormones. They act on nearly every part of the body.
Hypopituitarism is when there isn't enough of one or more of the pituitary hormones. This lack of hormones, called a deficiency, can affect how the body works in many ways. These include growth, blood pressure and the ability to have children, among others. Symptoms depend on which hormones are missing.
People who have hypopituitarism usually need to take medicines for the rest of their lives. These medicines replace the missing hormones, which helps control symptoms.
Symptoms
The symptoms of hypopituitarism usually start slowly and get worse over time. They might not be noticed for months or even years. But for some people, symptoms start suddenly.
Symptoms of hypopituitarism vary from person to person. Symptoms depend on what hormones are missing and how little of the hormone is being made. There might be more than one hormone that's low. A second hormone deficiency might increase the symptoms of the first one. Or sometimes, it might hide those symptoms.
Growth hormone (GH) deficiency
In children, GH deficiency can cause growth problems and short stature. Most adults who have GH deficiency don't have symptoms. But some adults have:
- Fatigue.
- Muscle weakness.
- Changes in body fat.
- Loss of interest in activities.
- Lack of social contacts.
Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) deficiency
A lack of these hormones, called gonadotropins, affects the reproductive system.
The lack of hormones keeps the ovaries from making enough eggs and estrogen. It keeps the testicles from making enough sperm and testosterone. This can lower sex drive and cause tiredness. It also can make it hard or impossible to have children — a condition called infertility. In children, the physical changes to an adult body, known as puberty, may not occur or may be late.
Some people might have symptoms such as:
- Hot flashes.
- Irregular periods or no periods.
- Loss of pubic hair.
- Not being able to make milk for breastfeeding.
- Not being able to get or keep an erection, known as erectile dysfunction.
- Decreased facial or body hair.
- Mood changes.
- Fatigue.
Thyroid-stimulating hormone (TSH) deficiency
This hormone controls the thyroid gland. Too little TSH leads to low levels of thyroid hormones. This condition is called hypothyroidism. It causes symptoms such as:
- Tiredness.
- Weight gain.
- Dry skin.
- Constipation.
- Sensitivity to cold or trouble staying warm.
Adrenocorticotropic hormone (ACTH) deficiency
This hormone helps the adrenal glands work correctly. It also helps the body react to stress. Symptoms of ACTH deficiency include:
- Severe tiredness.
- Low blood pressure.
- Many and lasting infections.
- Nausea, vomiting or abdominal pain.
- Confusion.
Anti-diuretic hormone (ADH) deficiency
This hormone, which also is called vasopressin, helps the body balance its fluid levels. An ADH deficiency can lead to a disorder called diabetes insipidus, which can cause:
- Urinating more than usual.
- Extreme thirst.
- Imbalances in minerals such as sodium and potassium, known as electrolytes.
Prolactin deficiency
Prolactin is the hormone that tells the body when to start making breast milk. Low levels of prolactin can cause problems with making milk for breastfeeding.
When to see a doctor
See your health care provider if you develop any symptoms of hypopituitarism.
Contact your health care provider right away if symptoms of hypopituitarism start suddenly or come with a bad headache, changes in vision, confusion or a drop in blood pressure. These could be symptoms of sudden damage to the pituitary gland tissue. This condition is known as pituitary apoplexy.
Bleeding into the pituitary gland can cause pituitary apoplexy. Pituitary apoplexy is a medical emergency and needs medical attention quickly.
Causes
Hypopituitarism has a number of causes. One common cause is a tumor of the pituitary gland. As a pituitary tumor grows, it can press on and damage pituitary tissue. This disrupts the pituitary gland's ability to make hormones. A tumor also can press on the optic nerves, causing vision problems.
Other potential causes of damage to the pituitary gland that may lead to hypopituitarism include:
- Lack of blood flow to the brain or pituitary gland, known as a stroke, or bleeding, called hemorrhage, into the brain or pituitary gland.
- Certain medicines, such as narcotics, high-dose steroids or certain cancer medicines called checkpoint inhibitors.
- Swelling, known as inflammation, of the pituitary gland caused by an unusual immune system response, called hypophysitis.
- Infections of the brain, such as meningitis, or infections that can spread to the brain, such as tuberculosis or syphilis.
- Significant blood loss during childbirth, which can damage the front part of the pituitary gland. This condition is known as Sheehan syndrome or postpartum pituitary necrosis.
In some cases, a change in a gene causes hypopituitarism. That change is heredity, which means it is passed down in families. The genetic change affects the pituitary gland's ability to make one or more of its hormones. This often starts at birth or in early childhood.
Tumors or diseases of a part of the brain that's just above the pituitary, called the hypothalamus, also can cause hypopituitarism. The hypothalamus makes hormones that affect how the pituitary gland works.
Sometimes, the cause of hypopituitarism isn't known.
Risk factors
Most people with hypopituitarism don't have any factors that put them at higher risk of developing the condition. But the following may raise the risk of developing hypopituitarism:
- A head injury.
- Brain surgery.
- Radiation treatment to the head or neck.
- Diseases that affect more than one part of the body. These include an inflammatory disease that affects various organs, called sarcoidosis; a disease in which unusual cells cause scarring, called Langerhans cell histiocytosis; and a disease that causes too much iron in the liver and other tissues, called hemochromatosis.
Diagnosis
Several tests can check hormone levels in the body and look for the cause of problems with the way the pituitary is working. These include:
- Blood tests. These tests measure levels of the hormones made in the pituitary gland and those made in glands that the pituitary controls, such as the thyroid gland. Blood tests can show if low hormone levels are due to the pituitary not working as it should.
- Stimulation or dynamic testing. A clinic that specializes in endocrine conditions can run these tests to measure hormone levels. These tests check the body's hormone levels before and after taking medicines that cause the body to make hormones.
- Brain imaging. MRI or CT scans of the brain can show a pituitary tumor or other pituitary gland problems.
Treatment
Hypopituitarism is treated with medicines that raise hormone levels. This is called hormone replacement. Doses are set to match the amount of hormones that the body would make if it didn't have a pituitary problem. In some cases, people with hypopituitarism may need to take this medicine for the rest of their lives.
Sometimes, treatment of a condition causing hypopituitarism may restore the body's ability to make pituitary hormones, either fully or in part.
Medications
Hormone replacement medicines might include:
- Cortisol replacement. These medicines include hydrocortisone (Cortef) or prednisone (Rayos). Taken by mouth, they replace the adrenal hormones needed because of a lack of adrenocorticotropic hormone (ACTH).
- Levothyroxine (Levoxyl, Synthroid, others). This medicine treats the low thyroid hormone levels, known as hypothyroidism, from a lack of thyroid-stimulating hormone (TSH).
- Sex hormones. These include testosterone, estrogen and progesterone. Testosterone is given by a shot, pills, patch or gel. Estrogen and progesterone usually are given in pills, gels or patches.
- Growth hormone. Also called somatropin (Genotropin, Humatrope, others), growth hormone is given by a shot under the skin. It promotes growth, which helps children grow taller. Adults who lack growth hormone also can benefit from growth hormone, but they won't get taller.
- Fertility hormones. Gonadotropins can be given by a shot to help ovulation and sperm production.
Monitoring hormone replacement
A specialist in endocrine disorders, called an endocrinologist, may keep an eye on symptoms and hormone levels in the blood. This is to ensure that the right amount of medicine is given.
People who take cortisol replacement need to work with a health care provider to adjust the dose during times of major stress. Under stress, the body usually makes extra cortisol to help manage the stress.
Having the flu, diarrhea or vomiting, or having surgery or dental work might mean the dose needs to be changed. The same might be true during pregnancy or with big changes in body weight.
Surgery or other procedures
If a tumor in or around the pituitary gland is the cause of hypopituitarism, surgery might be needed to remove the growth. Some tumors also can be treated with medicines or radiation therapy.
In case of emergency
People with hypopituitarism need to wear a medical alert bracelet or necklace and carry a card telling others of the condition. This is especially important for those taking cortisol replacement for a lack of ACTH.
Preparing for an appointment
You're likely to start by seeing your primary care provider. Sometimes, you might be referred to a specialist in endocrine disorders, known as an endocrinologist.
Here's some information to help you get ready for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do to get ready for tests you may need.
- Write down all symptoms you have, even if they seem not to be linked to each other. Note when they began.
- Write down key personal information, including any recent life changes or a change in your ability to cope with stress.
- Make a list of your key medical information, including recent surgeries and any other conditions for which you've been treated. Write down the names of all medicines you take, including doses. List injuries to your head or problems during childbirth.
- Take a family member or friend along, if possible. Someone who accompanies you can help you remember what your care provider tells you.
- Write down questions to ask your care provider.
Create a list of questions before your appointment so that you can make the most of your time with your provider. For hypopituitarism, some basic questions to ask include:
- What is likely causing my symptoms?
- What are other possible causes?
- What tests do I need?
- Is my condition likely to be short-term or long-term?
- What treatment do you recommend?
- How long will I need to take medicines?
- How will you know if my treatment is working?
- I have other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- Do you have brochures or other printed material I can have? What websites do you recommend?
Be sure to ask all the questions you have.
What to expect from your doctor
Your care provider might ask questions, such as:
- How have your symptoms changed over time?
- Has your vision changed?
- Do you have bad headaches?
- Has your weight or the amount of your body hair changed? Are there other changes in how you look?
- Have you lost interest in sex? Has your menstrual cycle changed?
- Have you recently had a baby?
- Have you had a head injury or neurosurgery?
- Have you ever had radiation treatment for a head or neck tumor?
- Have any of your family members been diagnosed with pituitary or hormonal conditions?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


