Overview
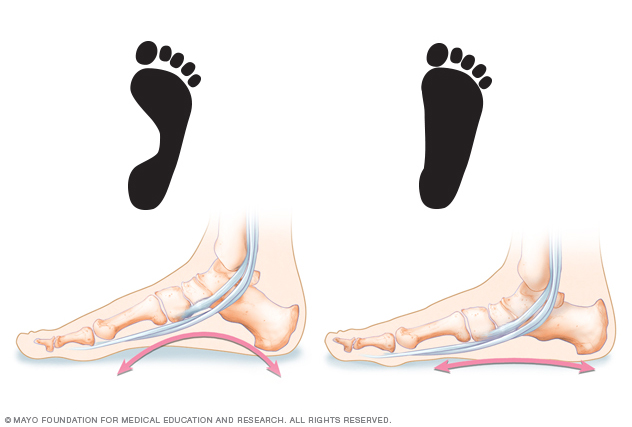
Flatfeet is a common condition, also known as flatfoot, in which the arches on the inside of the feet flatten when pressure is put on them. When people with flatfeet stand up, the feet point outward, and the entire soles of the feet fall and touch the floor.
Flatfeet can occur when the arches don't develop during childhood. It can also develop later in life after an injury or from the simple wear-and-tear stresses of age.
Flatfeet is usually painless. If you aren't having pain, no treatment is necessary. However, if flatfeet is causing you pain and limiting what you want to do, then an evaluation from a specialist may be warranted.
Symptoms
Most people have no symptoms associated with flatfeet. But some people with flatfeet experience foot pain, particularly in the heel or arch area. Pain may worsen with activity. Swelling may occur along the inside of the ankle.
When to see a doctor
Talk to your health care provider if you or your child has foot pain, particularly if it is limiting what you want to do.
Causes
Flatfeet is not unusual in infants and toddlers, because the foot's arch hasn't yet developed. Most people's arches develop throughout childhood, but some people never develop arches. People without arches may or may not have problems.
Some children have flexible flatfeet, often called flexible flatfoot, in which the arch is visible when the child is sitting or standing on tiptoes but disappears when the child stands. Most children outgrow flexible flatfeet without problems.
People without flatfeet can also develop the condition. Arches can collapse abruptly after an injury. Or the collapse can happen over years of wear and tear. Over time, the tendon that runs along the inside of the ankle and helps support the arch can get weakened or tear. As the severity increases, arthritis may develop in the foot.
Risk factors
Factors that can increase the risk of flatfeet include:
- Obesity
- Injury to the foot or ankle
- Rheumatoid arthritis
- Aging
- Diabetes
Diagnosis
To view the mechanics of your feet, a health care provider will observe your feet from the front and back and ask you to stand on your toes. The provider will test strength in the ankles and locate the main area of your pain. The wear pattern on your shoes also may reveal information about your feet.
Tests
Imaging tests that can be helpful in diagnosing the cause of foot pain may include:
- X-rays. A simple X-ray uses a small amount of radiation to produce images of the bones and joints in the feet. It's particularly useful in evaluating alignment and detecting arthritis.
- CT scan. This test takes X-rays of the foot from different angles and provides much more detail than a standard X-ray.
- Ultrasound. Ultrasound may be used when a tendon injury is suspected. Ultrasound uses sound waves to produce detailed images of soft tissues within the body.
- MRI. Using radio waves and a strong magnet, MRIs provide excellent detail of both bone and soft tissues.
Treatment
No treatment is necessary for flatfeet if it doesn't cause pain.
Therapies
For painful flatfeet, a health care provider might suggest:
- Arch supports (orthotic devices). Nonprescription arch supports can help relieve the pain caused by flatfeet. Sometimes custom-designed arch supports that are molded to the contours of the feet are recommended. Arch supports won't cure flatfeet, but they often reduce symptoms.
- Stretching exercises. Some people with flatfeet also have a shortened Achilles tendon. Exercises to stretch this tendon may help.
- Physical therapy. Flatfeet may contribute to overuse injuries in some runners. A physical therapist can provide exercises to strengthen the muscles and tendons in the feet and guidance to improve gait.
Surgery
Surgery isn't done solely to correct flatfeet. Surgery may be an option when patients have pain that still limits their activities after they have tried nonsurgical treatments. Surgery can repair the bone and tendon problems that are causing the pain.
Lifestyle and home remedies
If flatfeet causes you minor pain, you might want to try:
- Rest. Avoid activities that aggravate the condition. Participate in low-impact activities — such as walking, biking or swimming — rather than jumping and running activities.
- Arch supports. Arch supports that are available without a prescription might increase your comfort.
- Medications. Pain relievers that are available without a prescription, such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve) might help.
- Weight loss. Losing weight can reduce stress on the feet.
Preparing for an appointment
If your feet cause you significant pain, your health care provider may refer you to a doctor specializing in foot disorders, such as an orthopedic surgeon or a podiatrist.
What you can do
Wear your everyday shoes to your appointment so your health care provider can look at the wear patterns on the soles. Before the appointment, you might want to write answers to the following questions:
- When did you first notice problems with your feet?
- What other medical problems, if any, do you have?
- Do your parents or siblings have flatfeet?
- Have you ever injured your foot or ankle?
- What medications and supplements do you take regularly?
What to expect from your doctor
Your health care provider may ask some of the following questions:
- Where exactly does it hurt?
- How would you describe the pain — dull, sharp, burning?
- What makes the pain worse? What makes the pain better?
- Does the type of shoe you wear affect the pain?
- Have you tried arch supports?
- How does the pain affect your life?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


