Overview
Bone spurs are bony growths that form along bone edges. They're also called osteophytes. Bone spurs often form where bones meet each other — in the joints. They also can form on the bones of the spine.
The main cause of bone spurs is the joint damage linked with the most common type of arthritis. This is called osteoarthritis. Bone spurs often cause no symptoms. You might not notice them, and your healthcare team might not happen to find them for years. Bone spurs might not need treatment. If treatment is needed, it depends on where spurs are located and how they affect your health.
Symptoms
Often, bone spurs don't cause symptoms. You might not know you have bone spurs until an X-ray for another condition reveals the growths. But sometimes, bone spurs can cause pain and loss of motion in your joints.
The symptoms depend on where the bone spurs are. Examples include:
- Knee. Bone spurs in the knee can make it painful to extend and bend the leg.
- Spine. On the small bones that form the spine, bone spurs can narrow the space that contains the spinal cord. These bone spurs can pinch the spinal cord or its nerve roots. That can cause weakness or numbness in the arms or legs.
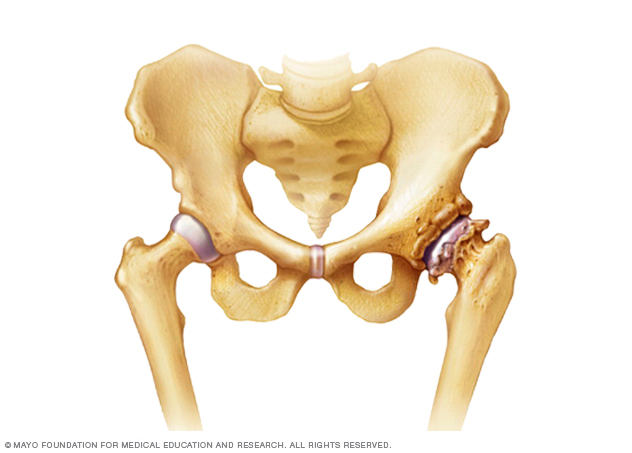
- Hip. Bone spurs can make it painful to move the hip. Sometimes, it might feel like the pain is in the knee or the thigh. Depending on their placement, bone spurs can reduce the range of motion in the hip joint.
When to see a doctor
Get a healthcare checkup if you have:
- Pain or swelling in one or more joints.
- Trouble moving a joint.
- Weakness or loss of feeling in the arms or legs.
Causes
Joint damage from osteoarthritis is the most common cause of bone spurs. Osteoarthritis breaks down connective tissue called cartilage that cushions the ends of bones. While this happens, the body tries to repair the loss by creating bone spurs near the damaged area.
Risk factors
The risk of bone spurs is higher in people who have arthritis.
Diagnosis
Your healthcare professional gives you a physical exam. Your doctor or another member of your healthcare team might feel around your joint to pinpoint your pain. X-rays or other imaging tests may be done to view your joints and bones.
Treatment
Medications
If you have bone spurs that cause pain, your healthcare professional might recommend pain relievers sold without a prescription. These include:
- Acetaminophen (Tylenol, others).
- Ibuprofen (Advil, Motrin IB, others).
- Naproxen sodium (Aleve, others).
Therapies
Physical therapy can help strengthen muscles around the joints. It also can help you become more flexible. This eases pain and helps you move better.
Surgery or other procedures
Some people with painful bone spurs due to osteoarthritis may benefit from surgery if other treatments don't work. Surgery might include removing bone spurs or replacing an affected joint. It depends on where the bone spurs are, how painful they are and how much they limit movement.
Lifestyle and home remedies
If you are overweight and have osteoarthritis of the hips or knees, weight loss may help ease bone spur pain. Even a small amount of weight loss may help.
Exercise can help people lose extra weight. It also can make muscles around joints stronger. Types of exercise that can help include walking, biking and swimming.
Preparing for an appointment
You'll likely first see your primary healthcare professional. You might be referred to a doctor who finds and treats joint conditions, called a rheumatologist.
Here's some information to help you get ready for your appointment.
What you can do
- List your symptoms and how long you've had them.
- Write down key medical information. Include any other conditions you have, all medicines and supplements you take, and any family history of bone or joint disease.
- Note recent injuries that affected a joint.
- Write down questions to ask your healthcare professional.
Here are some questions to ask your healthcare professional. Feel free to ask others.
- What's the most likely cause of my symptoms?
- Are there other possible causes?
- What tests do I need?
- What treatment do you recommend, if any?
- I have other health conditions. How can I manage them together?
- Is surgery an option for me? Why or why not?
- What self-care measures can I take to help manage symptoms?
What to expect from your doctor
Your healthcare professional is likely to ask you questions such as:
- How bad is your pain?
- Are you having trouble moving the affected joint or joints?
- Are your symptoms affecting your ability to complete daily tasks?
- If you've tried at-home treatments so far, what, if anything, has helped?
- What is your typical exercise routine?
© 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use


